Author(s): Wohlgemuth, Walter A.
Author(s): Wohlgemuth, Walter A.
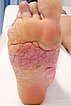
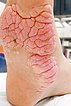
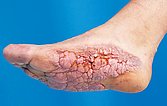
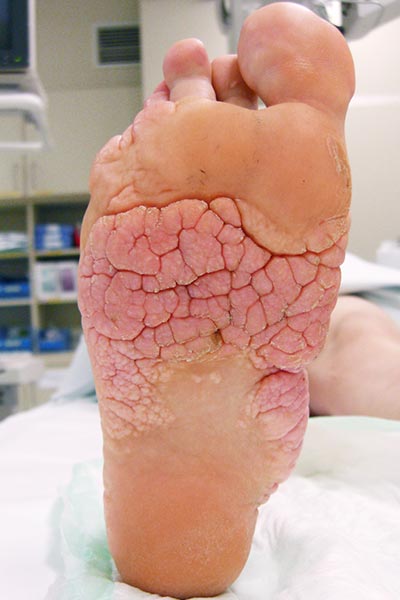
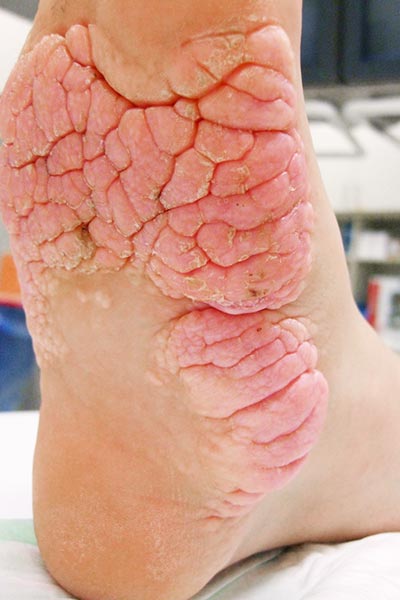
In this patient with Proteus syndrome, the classic so-called cerebriform mixed connective tissue nevus (CMCTN – on the foot also called “moccasin sole”), which is pathognomonic for the clinical picture, developed early on both soles of the feet.
The lesion is relatively hard on palpation and practically painless, growing very slowly. The surface somewhat resembles the surface of the brain, hence the name “cerebriform”. In the photograph the patient is 15 years old.
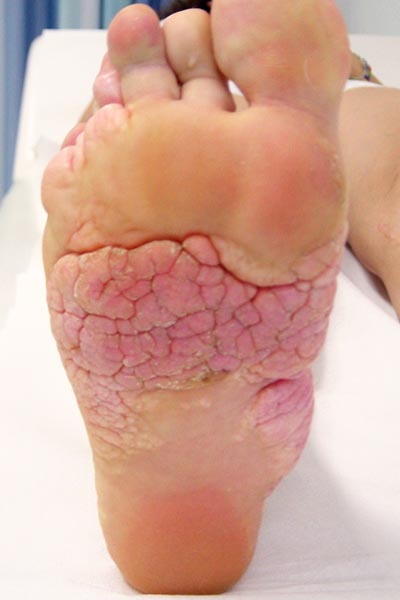
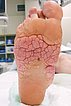
Almost exactly one year later (at the age of 16) the cerebriform mixed connective tissue nevus has enlarged a little at the medial edge of the foot. It causes the patient an unpleasant feeling of pressure when wearing shoes.
There is a wish for a surgical resection.
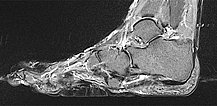
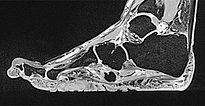
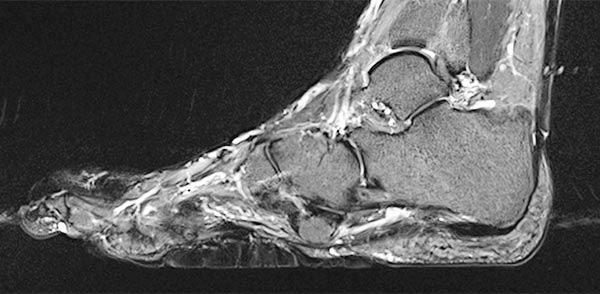
Preoperative imaging of the cerebriform mixed connective tissue nevus in MRI, here sagittal T2-weighted, fat-suppressed sequence of the right foot. The connective tissue nevus is homogeneously hypointense (black) due to the high fibrotic content.
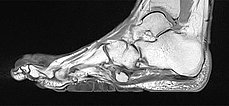
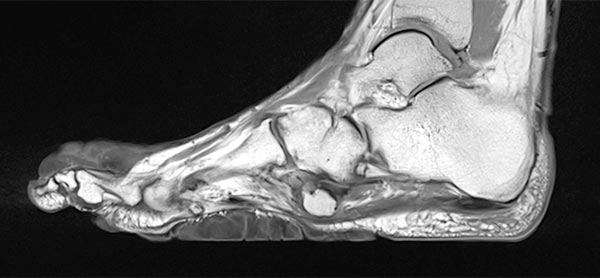
The cerebriform mixed connective tissue nevus is also homogeneously hypointense (black) on sagittal non-enhanced, T1-weighted MRI (same plane).
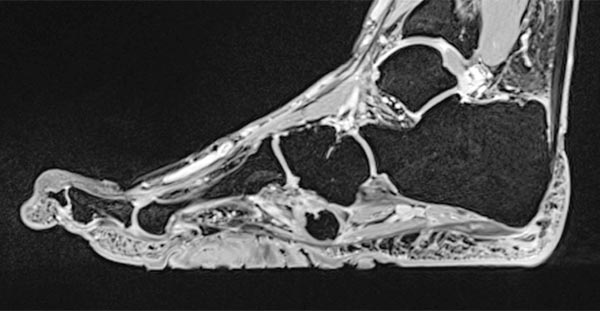
Sagittal , T1-weighted, fat-suppressed MRI (again, the same plane) shows slight, relatively homogeneous contrast enhancement of the nevus.
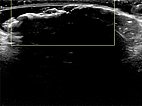
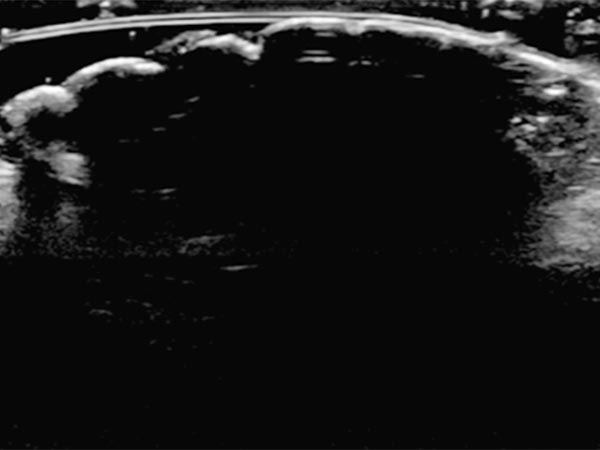
In sonography (B-scan), a total echo reflection with a pronounced acoustic shadow is found due to the high proportion of connective tissue on the surface of the nevus. The lesion itself cannot be visualized.
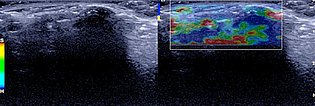
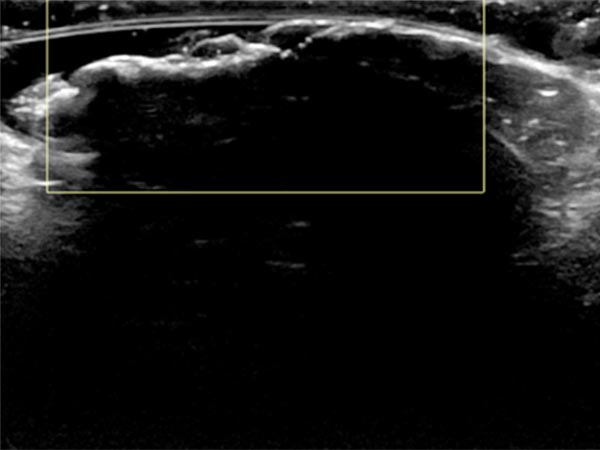
Color-coded duplex sonography also shows total echo reflection. No perfusion detectable even with a very sensitive setting for blood flow (6 cm/s).
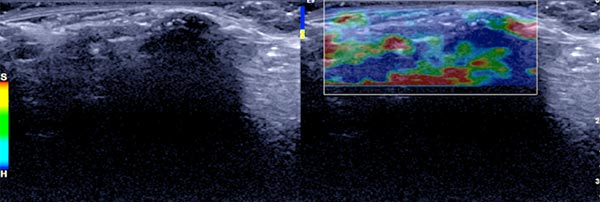
In ultrasound elastography, the lesion codes hard (blue) reflecting the high tissue hardness.
At almost 17 years of age, the medial portion of the connective tissue nevus slowly continues to increase. Finally, at the age of 18, the medial portion of the cerebriform mixed connective tissue nevus is surgically partially resected (not shown).
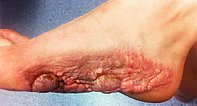
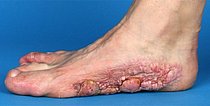
In the 20th year of life, about one and a half years after surgery, there is already clear recurrent growth of the cerebriform mixed connective tissue nevus at the resection site. Pearl-like, sometimes rather larger indurations form on the scar bed of the previous partial resection.
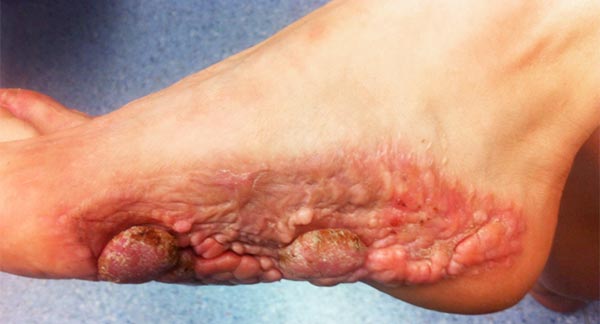
In the 21st year of life, further, slightly increasing recurrent growth of the cerebriform mixed connective tissue nevus is seen. Functionally, however, the result at this time is not bad, since the local pressure complaints are milder. However, as is common with this form of connective tissue nevus with greater extension, bacterial colonization of the crevices between the individual parts of the nevus occurs. Unpleasant inflammation can take place here.
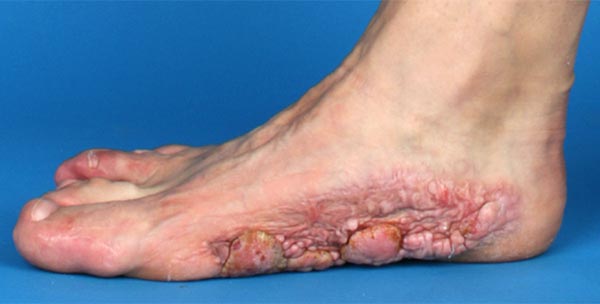
At 22 years of age, the recurrence is almost back to the same level of growth as before. Functionally, the result remained good. Recurrent bacterial inflammation occurs in the crevices between each elevated part of the lesion.
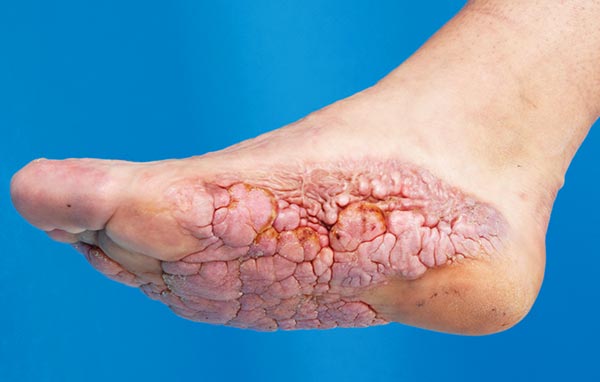
Cerebriform mixed connective tissue nevus (CMCTN) is a pathognomonic skin lesion on the soles of the feet or in some cases the palm that is virtually unique to Proteus syndrome. The lesion is characterized by very slowly progressive connective tissue proliferations whose surface looks like the surface of the brain (hence “cerebriform”). The tissue largely consists of connective tissue and is relatively hard. Surgical resection is difficult because, especially in the young growth years of Proteus patients, resecting too early may even result in exaggerated progressive recurrence. Overall, great restraint with regard to surgical measures is advisable in this situation.
The most important treatment method for CMCTN is to keep the crevices (“sulci”) between the individual exophytic parts (“gyri”) very clean and to disinfect them regularly, since the risk of bacterial infection is high even with strict cleanliness. These crevices can then be painful, plus the bacterial contamination can cause odor.
Published: 2020
All images © Wohlgemuth