Author(s): Wohlgemuth, Walter A.
Author(s): Wohlgemuth, Walter A.
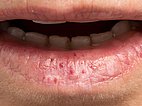
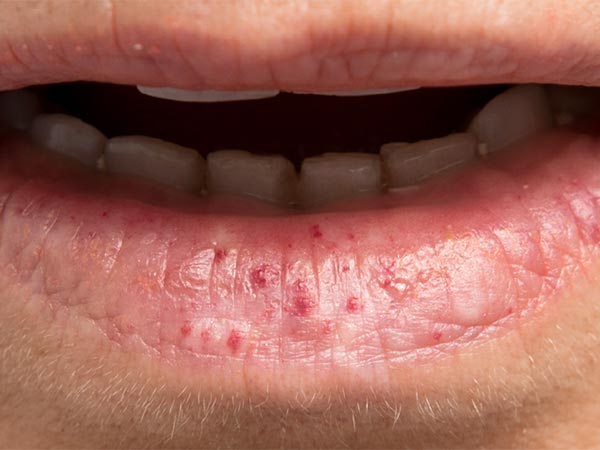
Patient with several small, cherry-red spots on the lower lip (Osler spots; teleangiectases) slowly progressing over the years. There has been recurrent nosebleed since childhood, also in the father and grandfather.
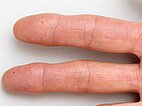
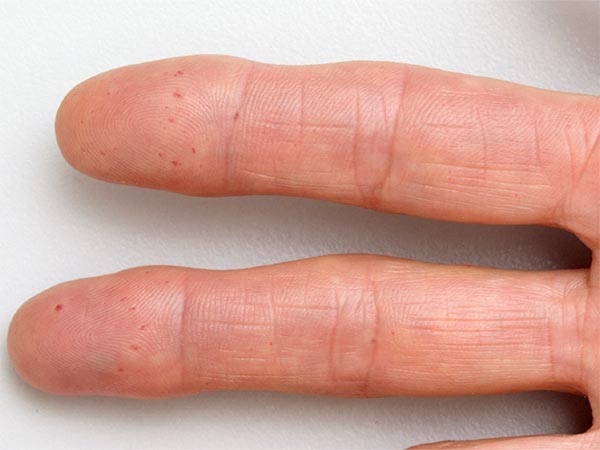
Similar small red, blood-filled spots (teleangiectases) have formed on the fingertips. They consist of dilated blood vessels (Osler spots).
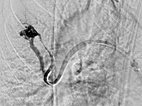
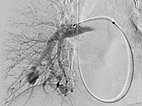
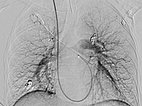
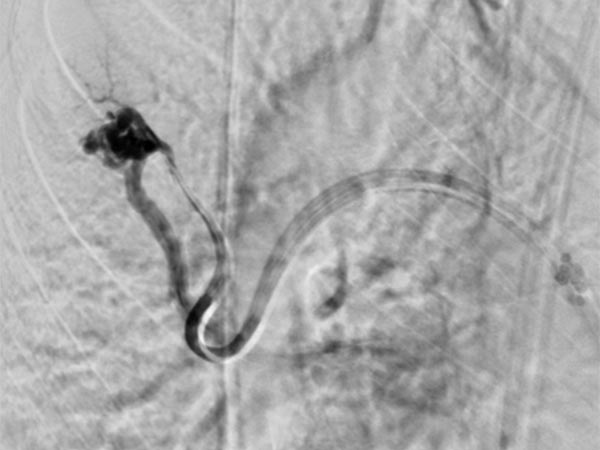
Upon evaluation of the underlying disease, contrast ultrasonography revealed a pulmonary right-to-left shunt, and computed tomography confirmed the finding of multiple pulmonary AVMs. Because of the size, there was an indication for embolization. Digital subtraction angiography demonstrates a pulmonary AVM in the upper lobe, already superselectively catheterized, with typical aneurysmally dilated arteriovenous shunt.
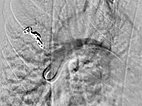
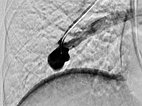
Occlusion of the pulmonary AVM of the upper lobe by insertion of multiple platinum wire loops (coils) via a microcatheter while sparing non-pathological pulmonary arteries.
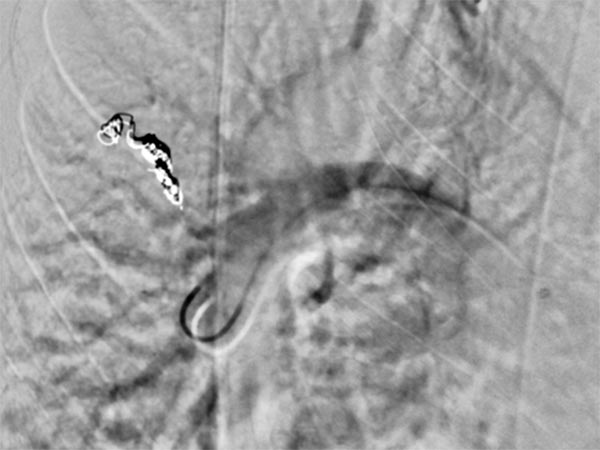
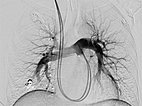
A guiding sheath was inserted into the right pulmonary artery from the neck (transjugular) via the heart, and a coaxial catheter was inserted through this by the Seldinger technique. After injection of contrast medium, pulmonary AVMs are also seen in the right lower lobe of the pulmonary circulation.
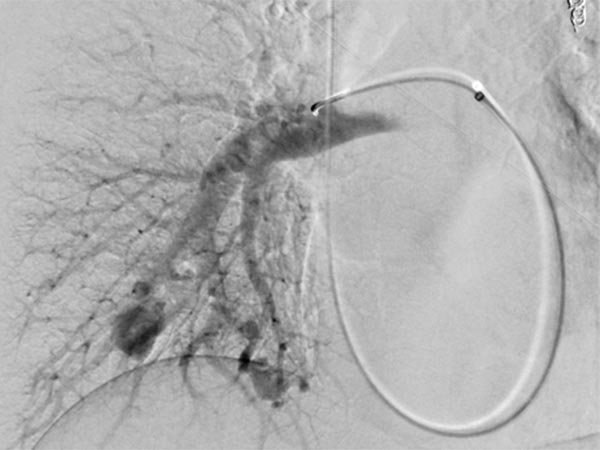
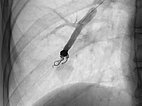
After cannulization of the larger pulmonary AVM, dilatation of the direct arteriovenous communication in the form of an aneurysm is seen. This is typical of Osler’s disease. The venous outflow is dilated, thus the risk of thromboembolism is particularly high.
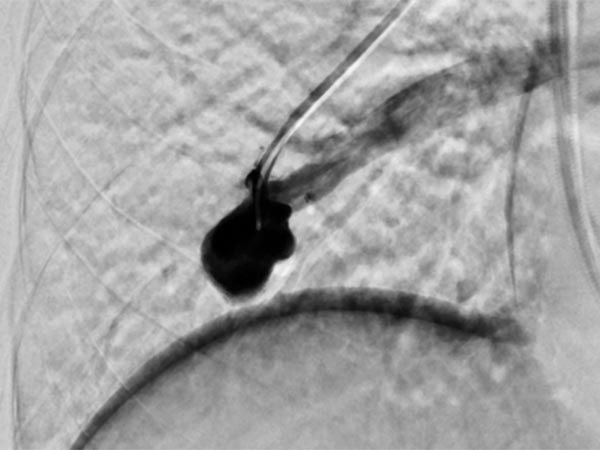
The feeding arteries are occluded with several coils. Parts of the coils are placed in the arterial feeding branch for secure anchoring (anchor technique). The pulmonary AVM is occluded. In the former aneurysm there is still some contrast medium stasis from a previous injection.
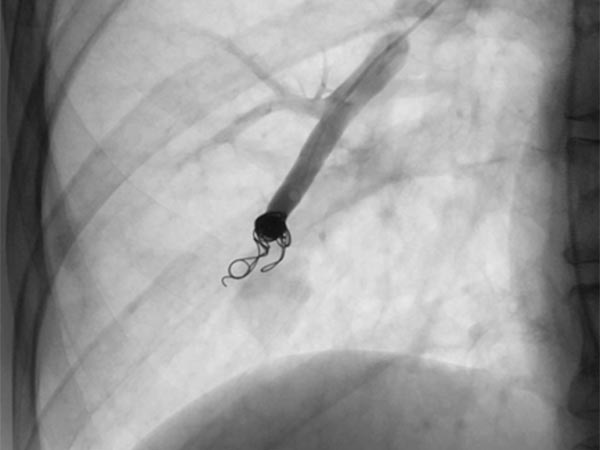
Completion DSA via the pulmonary trunk shows no more flow into the pulmonary AVMs.
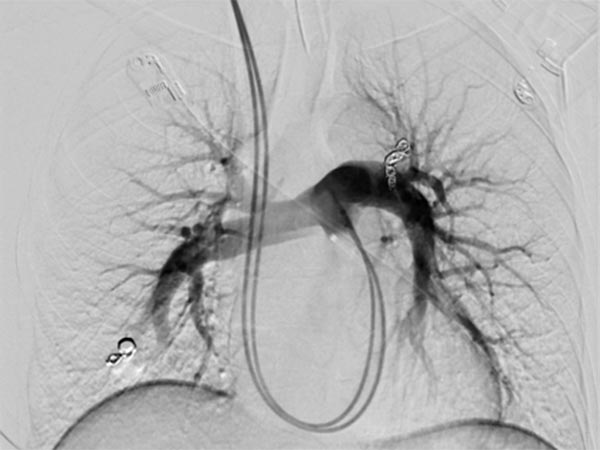
Completion DSA via the pulmonary trunk in the parenchymal phase confirms complete occlusion of the pulmonary AVMs.
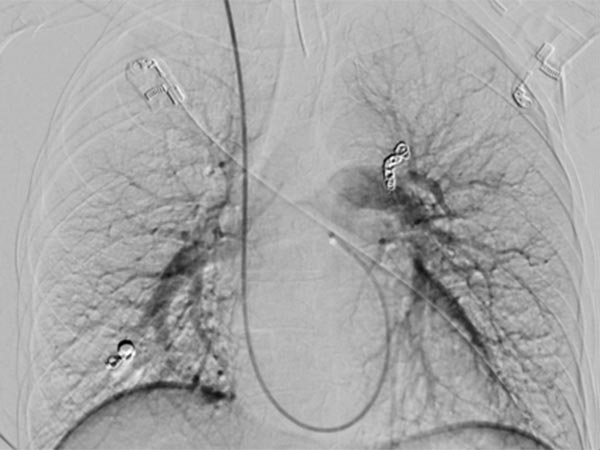
Patient with recurrent nosebleeds since 6 years of age. Positive family history (father, grandfather), no major problems in 2 pregnancies. No gastrointestinal symptoms, liver without pathological findings, no neurological symptoms so far. Multiple larger pulmonary AVMs were found in a recent chest computed tomography. A sonographically (CEUS) measured 24% right-left shunt with loss of filtering function of the pulmonary circulation for bacteria (septic embolisms) and for thrombi (arterial embolisms, also cerebral). Thus, there is a clear clinical risk to this patient, especially with regard to stroke.
Nowadays, this is a good indication for interventional occlusion of these pulmonary AVMs, which are typically markedly dilated in the region of the direct arteriovenous communication, in the form of aneurysms. This was very successful in this patient. She is on a long-term follow-up program to safely rule out recurrence or formation of new pulmonary AVMs.
Published: 2018
All images © Wohlgemuth