Author(s): Wohlgemuth, Walter A.
Author(s): Wohlgemuth, Walter A.
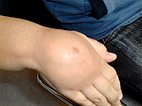
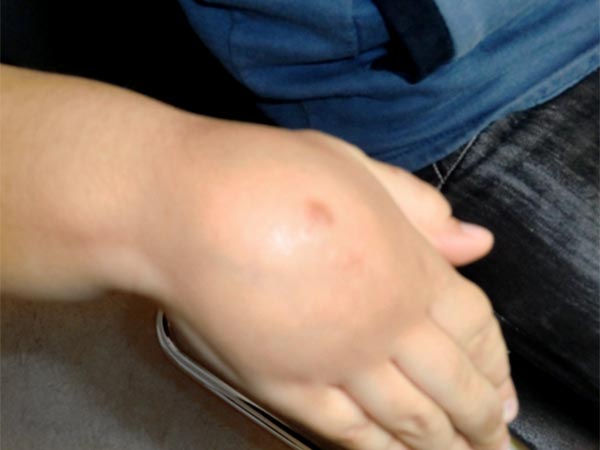
8-year-old boy with a non-discolored swelling on the dorsum of the right hand present since birth. On palpation it feels soft and elastic like a pillow and is moderately painful. Pain in response to touch rather than exertion (the boy is right-handed).
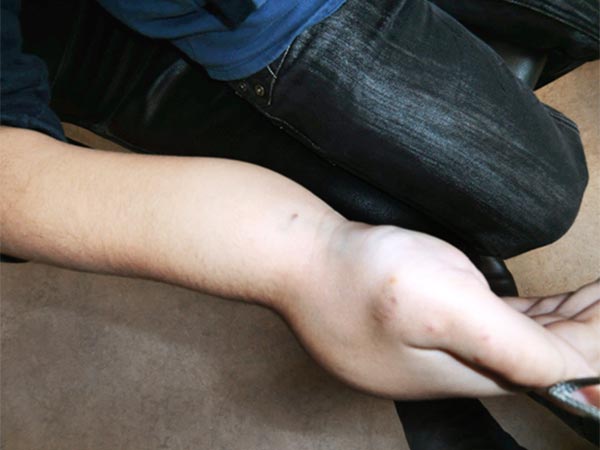
Similar soft palpable, sometimes painful swelling on the volar side of the distal right forearm.
Again, no bluish discoloration of the lesion, as is often seen in venous malformations.
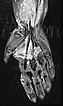
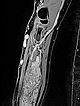
The coronal, T2-weighted, fat-suppressed sequence of an MRI with imaging of the right upper and lower arm shows a much larger extension of the malformation than clinically suspected.
The extension is predominantly subfascial in the depth of the muscles of the upper and lower arm. The signaling is strongly hyperintense, thus certainly a slow-flow malformation (venous or lymphatic).
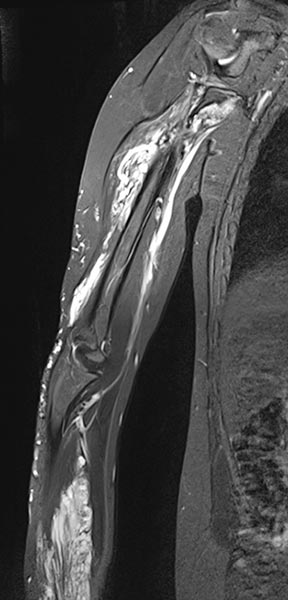
The venous malformation shows deep extension in the deep flexor tendons of the hand and forearm on T2-weighted, fat-suppressed MRI.
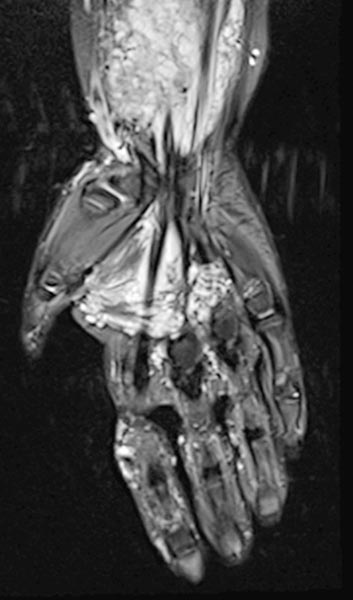
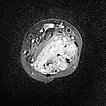
On the distal right forearm in the area of the main extension of the swelling, the bulk of the venous malformation is seen predominantly in the flexor muscles. Severely hyperintense MRI signal in T2w fat saturation. The entire flexor muscles are intermingled.
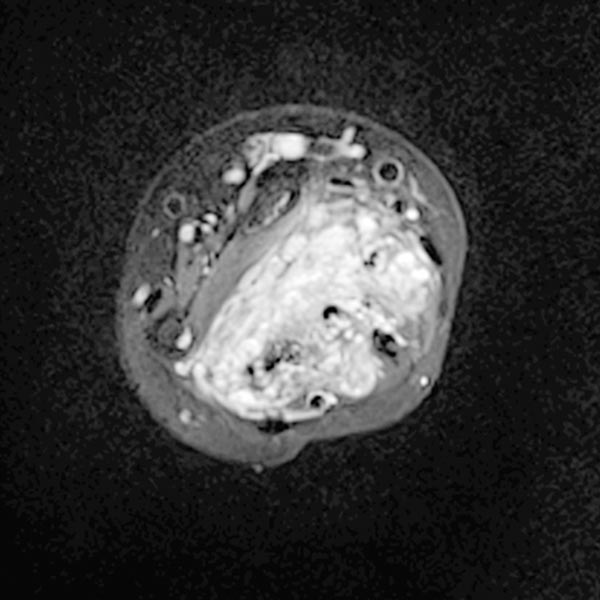
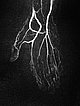
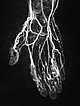
Dynamic, contrast-enhanced MR angiography of the hand, 30 s after intravenous contrast injection.
Normal hand arteries, no fast-flow situation, no dilated arteries or arteriovenous shunts are demonstrated.
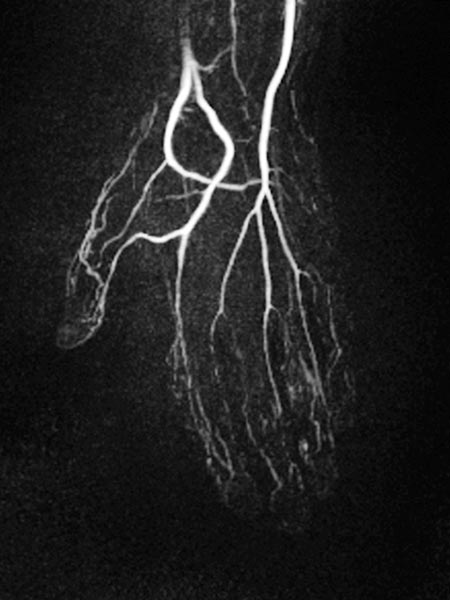
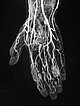
Dynamic, contrast-enhanced MR angiography of the hand, 35 s after contrast injection.
Already in this early arterial phase, first enhancement of parts of the malformation via small arteriovenous fistulas (AVF) mainly in thumb, index finger and ring finger.
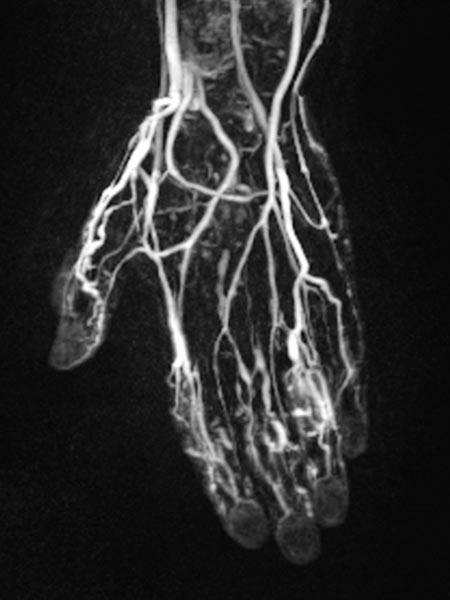
Dynamic, contrast-enhanced MR angiography of the hand, 67 s after contrast injection.
In this venous phase, slow pooling of contrast within the venous malformation.
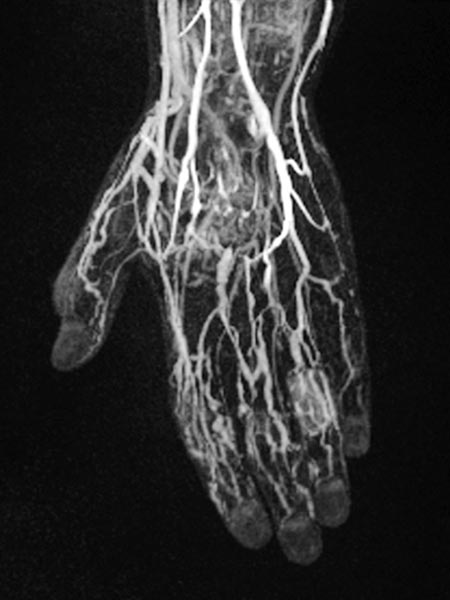
T1-weighted, fat-saturated, contrast-enhanced MRI sequence of the forearm.
The complete enhancement of the malformation in the musculature can clearly be seen. Therefore this is a venous malformation.
Some rather enlarged dysplastic veins are also found laterally on the proximal forearm epifascially in the subcutaneous fat tissue.
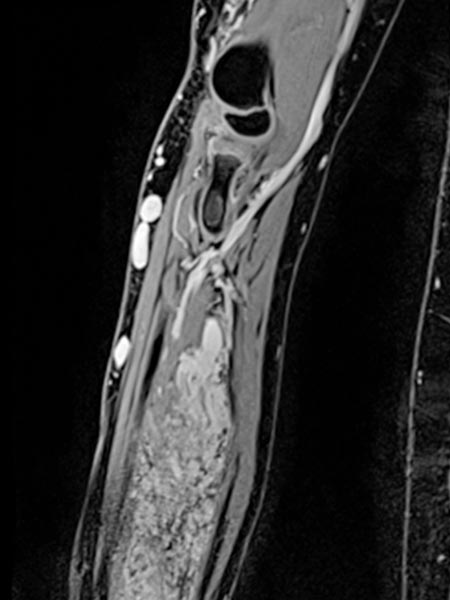
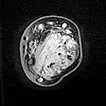
Axial T1-weighted, fat-suppressed contrast-enhanced sequence of the mid-forearm.
The venous malformation accumulates contrast within the involved muscle.
However, the vascular lumina of the venous malformation are relatively small, and no major tubular portions are found.
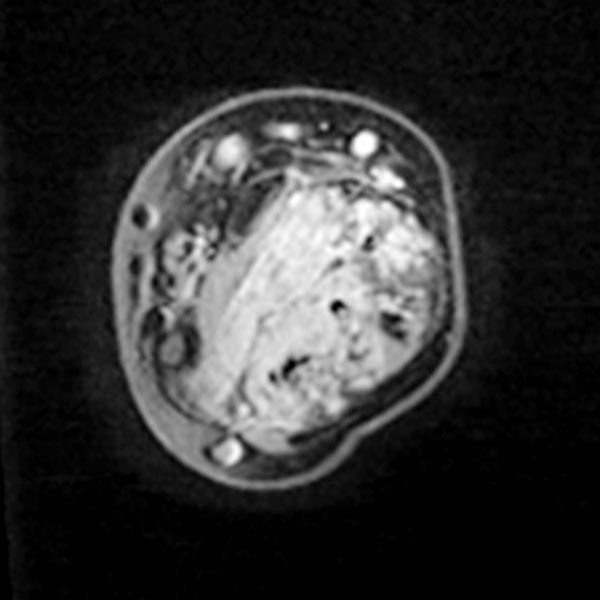
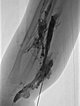
On account of the relatively small individual vessel diameters of the venous malformation, it is also difficult to puncture them directly. Varicography using a direct puncture technique shows multiple, rather elongated, partly reticular dysplastic small-lumen venous channels.
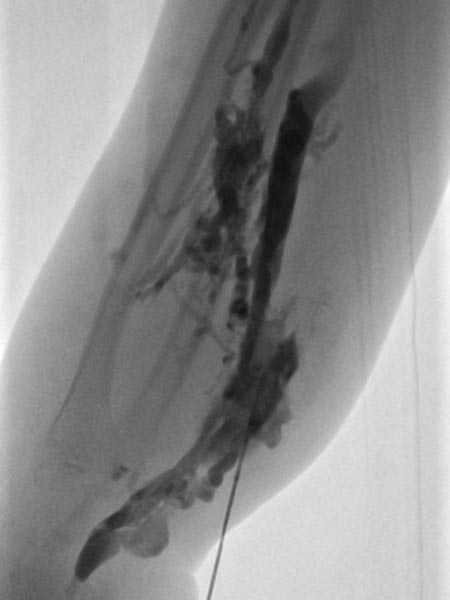
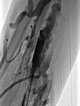
After the needle position is secured within the venous malformation and drainage via a major communicating vein is ruled out, polidocanol foam (3% Aethoxysklerol foamed 1 to 4 in air) is injected. This foam is not radiopaque but displaces the previously injected contrast material from the lesion.
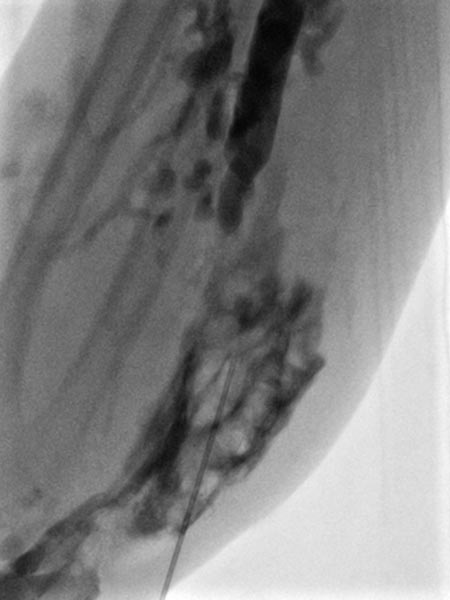
Further proximally in the forearm, the entire venous malformation in the depth of the flexor muscles is also gradually injected with sclerosing foam.
The procedure is repeated a total of 2 more times on the forearm and on the dorsum of the hand. On the forearm a good clinical result without persistent pain was achieved. On the back of the hand, however, pain persisted and the swelling did not decrease (in contrast to the forearm). Therefore, a local partial resection of the venous malformation was performed with good clinical results.
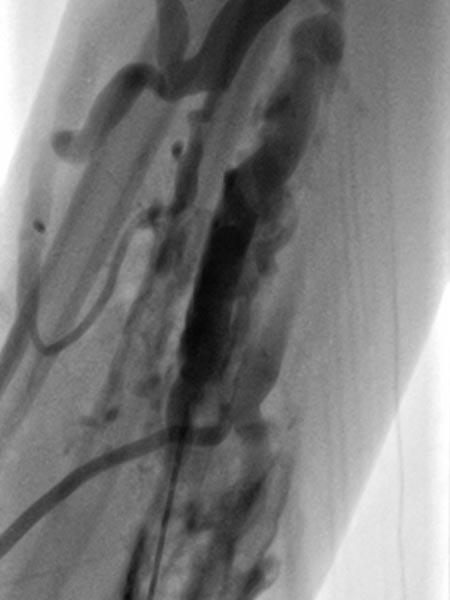
Extensive venous malformations of the extremity that completely penetrate the fine structures of the musculature and tendon compartments as well as the vascular nerve sheaths can hardly be treated curatively. Sclerotherapy alone is usually just as unsuccessful in the long term as attempts to resect them as completely as possible, which is technically hardly feasible. Therefore, combination therapy in several clearly pre-planned stages is the therapy of choice in this situation. The goal is not complete removal of the venous malformation, but elimination of the clinical symptoms.
Published: 2020
All images © Wohlgemuth